| Pathologist | With AI_1 | With AI_2 | With AI_3 | With AI_4 | With AI_5 | Without AI_1 | Without AI_2 | Without AI_3 | Without AI_4 | Without AI_5 |
|---|---|---|---|---|---|---|---|---|---|---|
| P1 | 25.7 | 25.1 | 6.6 | 11.4 | 31.1 | 43.1 | 10.8 | 6.0 | 9.0 | 31.1 |
| P2 | 11.4 | 31.7 | 12.0 | 32.3 | 12.6 | 17.4 | 20.4 | 22.8 | 22.2 | 17.4 |
| P3 | 10.8 | 34.7 | 11.4 | 15.6 | 27.5 | 19.2 | 8.4 | 4.8 | 19.2 | 48.5 |
| P4 | 15.0 | 24.6 | 20.4 | 25.1 | 15.0 | 10.2 | 12.0 | 16.2 | 44.3 | 17.4 |
8 Clinical Impact Analysis
9 Clinical Impact Analysis
9.1 Gleason Grade Group Changes
Impact of AI on Gleason Grading
Analyzing whether AI assistance leads to clinically significant changes in Gleason grade group assignment, which directly affects treatment decisions.
9.1.1 Grade Group Distribution
Note for Pathologists: This table shows the distribution of Gleason Grade Groups (1-5) assigned by each pathologist with and without AI, highlighting shifts in grade assignment.
9.1.2 Grade Group Upgrading and Downgrading
Clinically Significant Grade Changes
Identifying cases where AI assistance led to grade group upgrading or downgrading. Upgrading (increasing grade) may indicate more aggressive management, while downgrading may avoid overtreatment.
Note for Pathologists: This table quantifies the frequency of grade upgrading (higher grade with AI) and downgrading (lower grade with AI).
| Pathologist | Change | Count | Percentage |
|---|---|---|---|
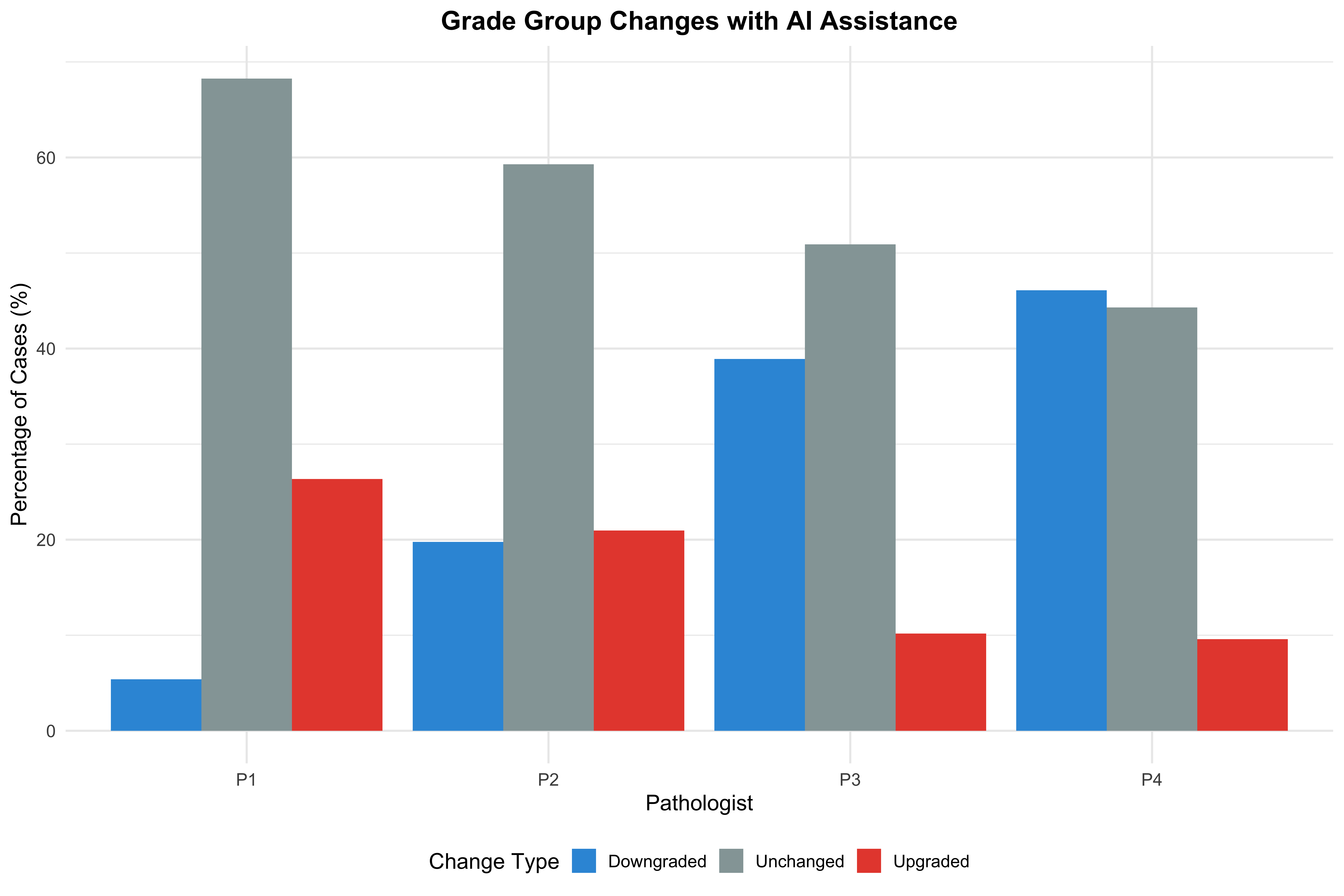
| P1 | Downgraded | 9 | 5.4 |
| P1 | Unchanged | 114 | 68.3 |
| P1 | Upgraded | 44 | 26.3 |
| P2 | Downgraded | 33 | 19.8 |
| P2 | Unchanged | 99 | 59.3 |
| P2 | Upgraded | 35 | 21.0 |
| P3 | Downgraded | 65 | 38.9 |
| P3 | Unchanged | 85 | 50.9 |
| P3 | Upgraded | 17 | 10.2 |
| P4 | Downgraded | 77 | 46.1 |
| P4 | Unchanged | 74 | 44.3 |
| P4 | Upgraded | 16 | 9.6 |
Note for Pathologists: Visual representation of the proportion of cases Upgraded, Downgraded, or Unchanged by each pathologist when using AI.
9.1.3 Clinical Significance of Grade Changes
Risk Category Reclassification
Analyzing changes in clinical risk categories based on grade groups: - Low Risk: Grade Group 1 - Intermediate Risk: Grade Groups 2-3 - High Risk: Grade Groups 4-5
Note for Pathologists: This analysis maps Grade Group changes to clinically significant Risk Categories (Low, Intermediate, High) to assess potential impact on patient management.
| Pathologist | Change | Count |
|---|---|---|
| P1 | Unchanged | 130 |
| P1 | Low Risk → Intermediate Risk | 29 |
| P1 | Intermediate Risk → High Risk | 6 |
| P1 | High Risk → Intermediate Risk | 2 |
| P2 | Unchanged | 132 |
| P2 | Low Risk → Intermediate Risk | 14 |
| P2 | Intermediate Risk → High Risk | 13 |
| P2 | High Risk → Intermediate Risk | 4 |
| P2 | Intermediate Risk → Low Risk | 4 |
| P3 | Unchanged | 107 |
| P3 | High Risk → Intermediate Risk | 40 |
| P3 | Low Risk → Intermediate Risk | 17 |
| P3 | Intermediate Risk → Low Risk | 2 |
| P3 | High Risk → Low Risk | 1 |
| P4 | Unchanged | 113 |
| P4 | High Risk → Intermediate Risk | 37 |
| P4 | Intermediate Risk → Low Risk | 12 |
| P4 | Low Risk → Intermediate Risk | 4 |
| P4 | Intermediate Risk → High Risk | 1 |
9.2 Tumor Detection Patterns
9.2.1 Small Tumor Detection
AI Performance on Small Tumor Foci
Evaluating AI’s ability to detect small tumor foci that might be missed by pathologists, stratified by tumor percentage.
Note for Pathologists: This table shows the detection of tumors of varying sizes (measured by percentage of core involvement) with and without AI.
| Pathologist | Count | With AI_Large (≥20%) | With AI_No Tumor | Without AI_Large (≥20%) | Without AI_No Tumor |
|---|---|---|---|---|---|
| P1 | 13 | 7.4 | 0.0 | 0.0 | 0.0 |
| P1 | 162 | 0.0 | 92.6 | 0.0 | 0.0 |
| P1 | 21 | 0.0 | 0.0 | 12.0 | 0.0 |
| P1 | 154 | 0.0 | 0.0 | 0.0 | 88.0 |
| P2 | 15 | 8.6 | 0.0 | 0.0 | 0.0 |
| P2 | 160 | 0.0 | 91.4 | 0.0 | 0.0 |
| P2 | 12 | 0.0 | 0.0 | 6.9 | 0.0 |
| P2 | 163 | 0.0 | 0.0 | 0.0 | 93.1 |
| P3 | 18 | 10.3 | 0.0 | 0.0 | 0.0 |
| P3 | 157 | 0.0 | 89.7 | 0.0 | 0.0 |
| P3 | 29 | 0.0 | 0.0 | 16.6 | 0.0 |
| P3 | 146 | 0.0 | 0.0 | 0.0 | 83.4 |
| P4 | 21 | 12.0 | 0.0 | 0.0 | 0.0 |
| P4 | 154 | 0.0 | 88.0 | 0.0 | 0.0 |
| P4 | 22 | 0.0 | 0.0 | 12.6 | 0.0 |
| P4 | 153 | 0.0 | 0.0 | 0.0 | 87.4 |
9.3 Impact on IHC and Consultation Requests
Reduction in Ancillary Testing
Quantifying the reduction in IHC requests and consultation needs when AI is available, indicating increased diagnostic confidence.
Note for Pathologists: This table compares the rate of ancillary test requests (IHC, Consultation) between the unassisted and AI-assisted workflows.
| Pathologist | AI_Status | IHC_Rate | Consult_Rate | Combined_Rate |
|---|---|---|---|---|
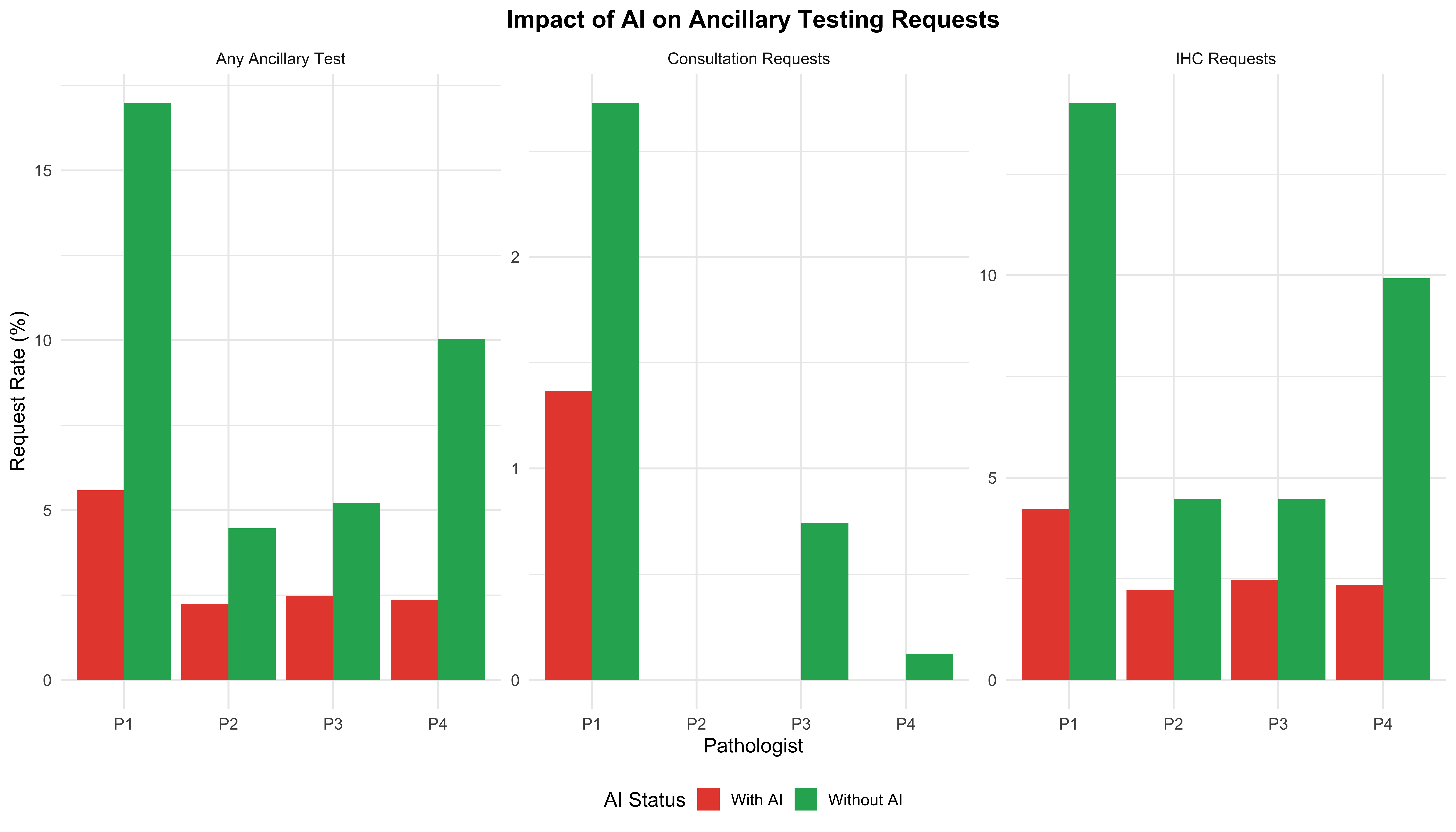
| P1 | Without AI | 14.3 | 2.7 | 17.0 |
| P1 | With AI | 4.2 | 1.4 | 5.6 |
| P2 | Without AI | 4.5 | 0.0 | 4.5 |
| P2 | With AI | 2.2 | 0.0 | 2.2 |
| P3 | Without AI | 4.5 | 0.7 | 5.2 |
| P3 | With AI | 2.5 | 0.0 | 2.5 |
| P4 | Without AI | 9.9 | 0.1 | 10.0 |
| P4 | With AI | 2.4 | 0.0 | 2.4 |
Note for Pathologists: Visual comparison of request rates for IHC, Consultation, and combined ancillary testing.
9.4 Summary of Clinical Impact
Key Clinical Findings
- Grade Group Changes: Quantification of upgrading and downgrading rates
- Risk Reclassification: Number of cases moving between risk categories
- Small Tumor Detection: AI impact on detecting minute tumor foci
- Ancillary Testing: Reduction in IHC and consultation requests
- Clinical Confidence: Overall improvement in diagnostic certainty
These metrics help quantify the real-world clinical utility of AI assistance in prostate biopsy diagnosis and its potential impact on patient management.
This chapter evaluates the clinical implications of AI-assisted diagnosis, focusing on Gleason grade changes, tumor detection patterns, and potential impact on patient management decisions.